Premenstrual Dysphoric Disorder (PMDD) is widely known for causing intense emotional and physical symptoms before menstruation. But what if the anxiety, mood swings, or fatigue don’t fully disappear even after your period ends?
Awareness Stage: What Is PMDD?
Premenstrual Dysphoric Disorder (PMDD) is a severe, hormone-sensitive mood disorder that occurs during the luteal phase of the menstrual cycle — typically 7–14 days before menstruation.
It is recognized in psychiatric and gynecological diagnostic guidelines as a legitimate medical condition, not simply “bad PMS.”
Common PMDD Symptoms (Before Period):
- Severe mood swings
- Depression or hopelessness
- Anxiety or panic attacks
- Irritability or anger
- Emotional sensitivity
- Brain fog
- Fatigue
- Sleep disturbances
- Bloating or breast tenderness
Classically, PMDD symptoms begin to improve within a few days after bleeding starts. However, some women report lingering symptoms even after their period ends.
Understanding the Hormonal Cycle
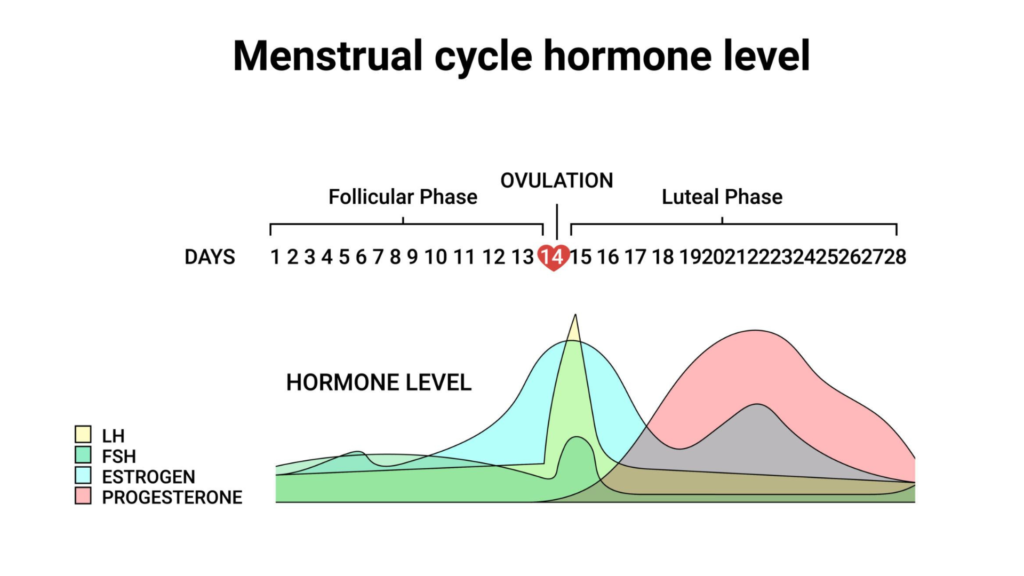
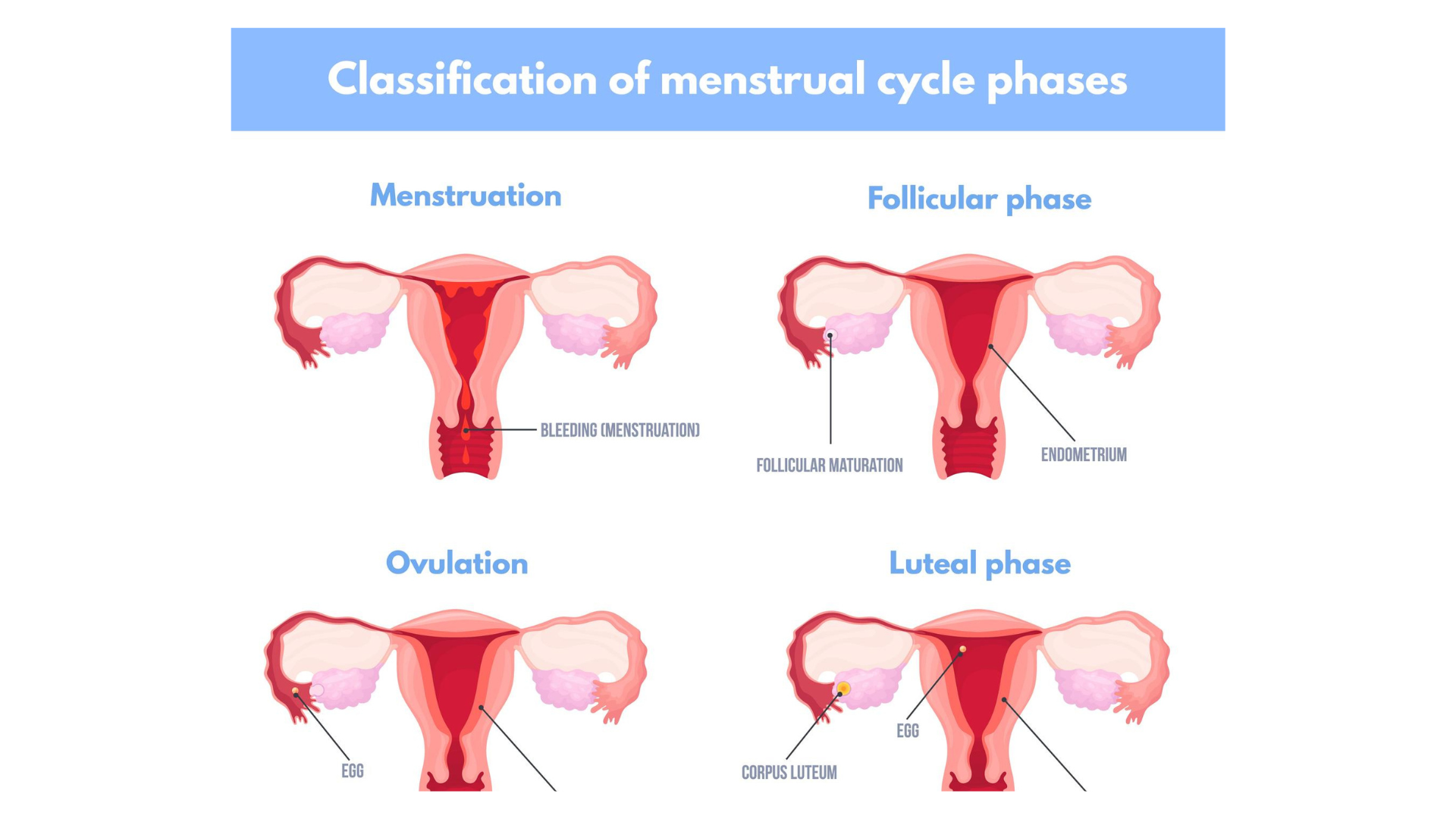

To understand lingering symptoms, we must understand hormone changes.
The menstrual cycle has four key phases:
- Menstrual Phase – Hormones are low; bleeding occurs.
- Follicular Phase – Estrogen gradually rises.
- Ovulation – Estrogen peaks.
- Luteal Phase – Progesterone rises; PMDD symptoms occur in sensitive individuals.
When your period begins, estrogen and progesterone drop sharply. After bleeding ends, estrogen starts rising again — but this stabilization is gradual, not immediate.
For women who are hormonally sensitive, even small fluctuations can affect mood.
Can PMDD Symptoms Continue After Period?
Technically, PMDD symptoms should resolve shortly after menstruation begins. If symptoms persist beyond that window, healthcare providers may reassess the diagnosis.
However, in real-world clinical patterns, some women experience:
- Emotional vulnerability
- Anxiety
- Mild depressive mood
- Mental fatigue
- Irritability
- Post-period exhaustion
- “Hormonal crash” feeling
This does not automatically mean your diagnosis is wrong. It means we must look deeper.
Consideration Stage: Why Symptoms May Continue After Your Period
1. Hormonal Transition Sensitivity



4
When menstruation starts, hormone levels are at their lowest. After bleeding, estrogen begins to rise.
For women with PMDD, the brain is particularly sensitive to hormonal shifts — not just high or low levels, but rapid changes.
This temporary adjustment period can cause:
- Mood instability
- Emotional sensitivity
- Irritability
- Fatigue
Hormonal stabilization may take several days.
2. Post-Menstrual Fatigue and Iron Deficiency
Post-menstrual fatigue is one of the most overlooked reasons women feel exhausted even after their period has ended. Many assume lingering tiredness is emotional or related to PMDD — but in some cases, it is physiological.
Why Does This Happen?
During menstruation, the body loses blood. Blood contains hemoglobin, a protein rich in iron that carries oxygen to tissues. When menstrual bleeding is heavy or prolonged, iron stores may temporarily drop.
If iron levels decline, the body struggles to deliver adequate oxygen to:
- The brain
- Muscles
- Organs
This reduced oxygen delivery directly impacts energy production.
Even mild iron deficiency (without full anemia) can cause noticeable symptoms.
How Iron Deficiency Causes Fatigue
Iron is essential for producing hemoglobin and supporting cellular energy (ATP production). When iron levels are low:
- Oxygen transport becomes inefficient
- Muscle endurance decreases
- Brain function slows
- Nervous system regulation weakens
This creates a feeling of:
- Persistent tiredness
- “Heavy” body sensation
- Slower thinking
- Emotional dullness
Unlike normal tiredness, post-menstrual fatigue may feel disproportionate to activity level.
Brain Fog and Cognitive Changes
Low iron affects neurotransmitters such as dopamine and serotonin, which regulate mood and concentration.
You may experience:
- Brain fog
- Difficulty concentrating
- Forgetfulness
- Slower decision-making
- Reduced motivation
This cognitive fatigue can mimic lingering PMDD symptoms.
Low Mood and Emotional Impact
Iron deficiency can contribute to:
- Irritability
- Mild depressive symptoms
- Emotional flatness
- Increased anxiety
This happens because iron plays a role in neurotransmitter synthesis. When iron is insufficient, emotional regulation may weaken.
Dizziness and Physical Weakness
Low hemoglobin reduces oxygen supply to muscles and the brain, leading to:
- Dizziness when standing
- Headaches
- Shortness of breath
- Paleness
- Cold hands and feet
If heavy periods are frequent, these symptoms may become cyclical.
Who Is at Higher Risk?
You may be more vulnerable if you:
- Have heavy menstrual bleeding (soaking a pad every 1–2 hours)
- Experience periods lasting more than 7 days
- Follow a low-iron diet
- Are vegetarian without iron planning
- Have underlying conditions like fibroids or PCOS
When to Consider Testing
If fatigue persists for several days after your period and is accompanied by:
✔ Dizziness
✔ Hair thinning
✔ Pale skin
✔ Brittle nails
✔ Shortness of breath
A simple blood test can check:
- Hemoglobin levels
- Serum ferritin (iron stores)
Ferritin is especially important because it shows stored iron — not just current circulating levels.
Supporting Recovery Naturally
To restore iron levels:
Include iron-rich foods such as:
- Spinach
- Lentils
- Chickpeas
- Beans
- Tofu
- Pumpkin seeds
Pair with Vitamin C sources (like lemon, oranges) to improve absorption.
Avoid consuming tea or coffee immediately after iron-rich meals, as they reduce absorption.
In moderate to severe deficiency, doctors may prescribe iron supplements.
Key Takeaway
Sometimes what feels like lingering PMDD is actually post-menstrual depletion.
Your body may not be emotionally unstable — it may simply be low on iron.
If fatigue is prominent after every cycle, iron evaluation is not overreacting — it is responsible health monitoring.
Understanding the difference between hormonal mood shifts and physiological depletion empowers you to seek the right solution.
3. Overlapping Mood Disorders
Here is your expanded section with a clear EEAT-based explanation (Expertise, Experience, Authority, Trustworthiness) added in a medically responsible tone:
If symptoms:
- Occur throughout the month
- Do not clearly improve after menstruation
- Affect daily functioning consistently
Doctors may evaluate for:
- Major Depressive Disorder (MDD)
- Generalized Anxiety Disorder (GAD)
- Persistent Depressive Disorder (Dysthymia)
PMDD can coexist with other mental health conditions.
Mental health professionals rely on:
- Structured diagnostic criteria
- Symptom tracking over at least two menstrual cycles
- Clinical interviews
- Functional impact assessment
This ensures accurate differentiation between:
- Hormone-triggered PMDD
- Ongoing depressive disorders
- Anxiety spectrum conditions
Why This Distinction Is Important
From a Trustworthiness perspective, accurate diagnosis determines proper treatment.
For example:
- PMDD often responds well to SSRIs taken cyclically or continuously.
- Major depressive disorder may require continuous psychiatric treatment.
- Anxiety disorders may benefit from therapy, stress regulation strategies, and medication.
Mislabeling persistent depression as PMDD can delay appropriate care.
Clinical Experience Insight
From clinical observation and research:
- PMDD and mood disorders can overlap.
- Women with existing depression may experience premenstrual worsening.
- Hormonal sensitivity can amplify underlying anxiety patterns.
This is why healthcare providers look for patterns — not just symptoms.
When to Seek Immediate Help
If you experience:
- Suicidal thoughts
- Severe hopelessness
- Panic attacks that interfere with daily functioning
- Inability to work, study, or maintain relationships
Immediate professional evaluation is essential.
Key Takeaway
PMDD is cyclical.
If emotional symptoms are persistent and not tied clearly to your menstrual phase, broader mental health evaluation is appropriate.
Seeking help is not overreacting — it is informed and responsible self-care.
Understanding the difference between cyclical hormonal mood shifts and ongoing mood disorders ensures you receive the right support and treatment.
4. Stress and Cortisol Imbalance
Chronic stress increases cortisol, which interacts with reproductive hormones.
High stress levels can:
- Prolong mood symptoms
- Disrupt sleep
- Worsen anxiety
- Delay emotional recovery after menstruation
Sleep deprivation during the luteal phase may also extend exhaustion into the post-period phase.
Action Stage: What You Can Do
1. Track Symptoms for 2–3 Cycles
Cycle tracking is one of the most reliable tools.
Record:
- When symptoms begin
- When bleeding starts
- When symptoms improve
- Severity level (1–10 scale)
If symptoms clearly follow the luteal phase and fade gradually, PMDD remains likely. If they persist all month, further evaluation is necessary.
2. Support Hormonal Stability Through Nutrition
Balanced nutrition supports mood regulation.
Focus on:
- Protein-rich meals
- Iron-rich foods (spinach, lentils, beetroot, beans)
- Omega-3 fatty acids
- Hydration (2–3 liters daily)
Limit:
- Excess caffeine
- Refined sugar
- Ultra-processed foods
Stable blood sugar supports emotional stability.
3. Regulate Stress



4
Stress directly impacts hormonal sensitivity.
Helpful practices:
- Gentle yoga (Butterfly Pose, Supine Twist, Child’s Pose)
- 10-minute deep breathing
- Consistent sleep schedule
- Reducing screen time before bed
Even small stress-reduction habits can reduce symptom intensity.
Seek Professional Treatment When Needed
Evidence-based treatments for PMDD include:
- SSRIs (Selective Serotonin Reuptake Inhibitors) – Often first-line treatment
- Hormonal therapy (including certain birth control formulations)
- Cognitive Behavioral Therapy (CBT)
- Nutritional supplementation (Magnesium, Vitamin B6 — under supervision)
- Iron supplementation if deficient
PMDD is highly treatable.
It include:
- Severe depression
- Suicidal thoughts
- Loss of daily functioning
Immediate medical care is essential.
EEAT: Why This Information Is Trustworthy
This article is based on:
- Diagnostic criteria for PMDD recognized in psychiatric manuals
- Endocrinology research on estrogen and progesterone fluctuation
- Clinical treatment guidelines for PMDD
- Evidence-based menstrual health practices
PMDD is a recognized neuro-hormonal condition, not a personality issue or emotional weakness.
Reliable management requires medical evaluation — not self-blame.
Decision Stage: When Should You Consult a Doctor?
You should seek professional help if:
✔ symptoms last more than 3–5 days after menstruation
✔ Emotional symptoms affect work, relationships, or studies
✔ You cannot clearly identify a cyclical pattern
✔ Symptoms worsen over time
✔ You feel unsafe or overwhelmed
Early evaluation improves long-term outcomes.
Final Thoughts
PMDD usually improve once your period starts — but for some women, emotional or physical symptoms may linger briefly due to hormonal adjustment, fatigue, stress, or overlapping mood conditions.
Your menstrual cycle affects your brain as much as your body.
Persistent symptoms deserve medical attention, not dismissal.
With proper tracking, nutrition, stress management, and professional guidance, emotional stability is achievable.
You are not “overreacting.”
You are experiencing a hormone-sensitive condition that deserves care.
